Medford (541) 770-2020
Grants Pass (541) 956-2020
Email Us
Patient Portal
Your Eye Health
Your Health
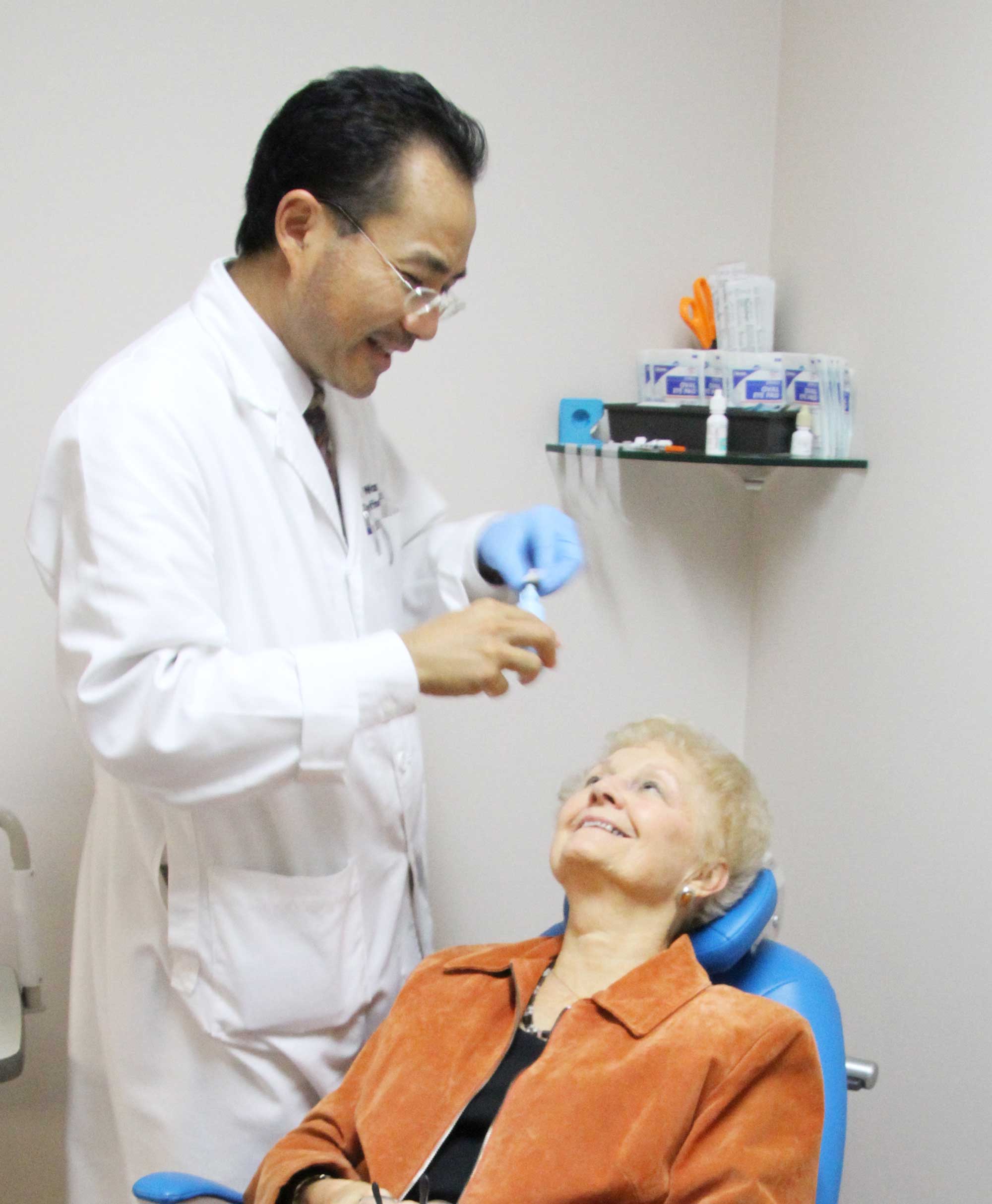
At Oregon Retina Center, Dr. Wang and our team will provide you with highly specialized medical and surgical eye and retina care. We specialize in eye conditions such as Diabetes, Macular Degeneration, and other retina disorders.
Conditions We Treat Include:
Age Related Macular Degeneration
Age-related macular degeneration is a condition that usually affects older adults. It results in a loss of vision in the center of the visual field due to retina damage. It occurs in “dry” and “wet” forms, making it difficult to read or recognize faces. However, enough peripheral vision remains to allow other activities of daily life.There are two types of AMD:
- Non-exudative (also known as dry AMD) is the most common form of the disease and has a better long-term visual prognosis than wet AMD. In the dry (nonexudative) form, cellular debris called drusen accumulates between the retina and the choroid, and the retina can become detached.
- Exudative (also known as wet AMD) is associated with the development of new blood vessels that grow beneath the retina leading to bleeding, scarring, and severe reduction in central vision. In the wet (exudative) form, which is more severe, blood vessels grow up from the choroid behind the retina, which can also become detached.
Diabetic Retinopathy
Diabetic retinopathy is damage to the retina caused by complications of diabetes, which can eventually lead to blindness. It is an ocular manifestation of systemic disease that affects up to 80% of all patients who have had diabetes for 10 years or more. Research indicates that at least 90% of these new cases could be reduced with proper and vigilant treatment and monitoring of the eyes. There are three primary treatments for diabetic retinopathy, which are very effective in reducing vision loss, including:
- Laser surgery
- Injection of corticosteroids or Anti-VEGF into the eye
- Vitrectomy
Retinal Detachments/Tears
The retina may tear or form holes as we undergo natural changes. The vitreous gel liquifies and suddenly pulls away from the retina, which may cause the retinal tissue to break. Once a retinal defect is present, a retina detachment may occur.
A retina detachment occurs when the neurosensory retinal tissue separates from the underlying retinal pigment epithelium and the choroid in the back of the eye. Many times, it is associated with photopsia or worsening floaters. Retina detachments are diagnosed in a dilated eye examination.
The specific treatment used to reattach the retina includes injecting a gas bubble (pneumatic retinopexy) to support the retina while new tissue builds, cryosurgery that allows the retina to reattach itself, or sclera buckle, in which a silicone implant is inserted permanently around the eye to reduce tension on the retinal surface and allow reattachment.
Vascular Occlusion
Vascular occlusion is a sudden blockage of a blood vessel, usually with a clot. When it occurs in a major vein, it can cause deep vein thrombosis. The condition is common in the retina and can cause partial or total loss of vision. An occlusion can often be diagnosed using Doppler sonography (a form of ultrasound). Occlusion can be carried out using a ligature; by implanting small coils which stimulate the formation of clots; or, particularly in the case of cerebral aneurysms, by clipping.
Macular Hole
A small central break in the macula tissue of the retina at the back of the eye is called a macular hole. If left untreated, it can lead to severe vision loss, including retinal detachment. If enough fibers connected to the vitreous separate over time, it can cause posterior vitreous detachment (PVD). When a PVD occurs, individuals may experience a sudden increase in Floaters. If the vitreous is firmly attached to the retina when it pulls away, it can create a Macular Hole. Once the macular hole is formed, it will cause blurred and distorted central vision.
In some cases, a small Macular Hole may close or heal on its own or need a surgical procedure known as a vitrectomy. During this procedure, your retinal specialist removes some of the vitreous gel and replaces it with a bubble of gas. The bubble helps close the Macular Hole and gradually dissolves over time.
Floaters and Flashes
Floaters appear as black spots or spider webs that seem to float in a cluster or individually within your vision. Flashes are flickering or flashing lights that are most prominent when you look at a bright background. With age, floaters can be caused by tiny bits of vitreous gel or cells that cast shadows on the retina. New floaters can sometimes be a sign of a more urgent retina problem. Flashes occur when the vitreous tugs on the sensitive retinal tissue. In some cases, floaters and flashes may be symptoms of more severe problems, such as retinal tears or retinal detachment. All patients who notice flashes or new floaters should seek immediate medical attention.
Epimacular Membrane
An epimacular membrane is a thin layer of tissue on the front surface of the macula. Decreased and distortion of central vision are the most common complaints by patients with an epimacular membrane. They do not cause total blindness. Most EMMs develop due to the separation of the vitreous (the jelly-like filling of the eye) from the macula. In rare cases, prior retinal freezing or laser procedures, retinal detachment surgery, or inflammatory and vascular diseases of the eye may be the contributing factors. Epimacular membranes typically develop in one eye, and over four to six weeks, most remain relatively stable after that. The only effective treatment is vitrectomy surgery and peeling of the membrane and ILM (internal limiting membrane).
Uveitis
Uveitis is an inflammation of the eye’s structures responsible for its blood supply. There are three major types of uveitis, each classified by the structures it affects.
1. Anterior uveitis affects the iris and ciliary body. Symptoms include light sensitivity, blurred vision, redness, pain, small pupils, and tearing.
2. Posterior uveitis involves the retina and choroid. Blurred vision and floaters are the most common symptoms.
3. Pan uveitis affects structures in both the front and back of the eye. It may have a combination of symptoms experienced with the other forms of uveitis.
Treatment is dependent on the severity of the disease and the ocular structures involved. Generally, topical eye drops and oral medications are prescribed to reduce inflammation. After the inflammation has been treated, the eye should be evaluated for secondary conditions, such as scar tissue, cataracts, or glaucoma.
Central/Branch Vein Occlusion
Central/Branch Artery Occlusion
Anterior Ischemia Optic Neuropathy (AION)
Endophthalmitis
Intraocular Lens Related Complications
Central Serous Chorioretinopathy (CSCR)
Ocular Trauma (Penetrating Eye Injuries)
Neovascular Glaucoma
Traumatic Cataract/Iris
Intraocular Tumors
Radiation Retinopathy
Hypertensive Retinopathy
Screening for Plaquenil Toxicity
Sickle Cell Retinopathy
All Diseases of the Vitreous, Macula, or Retina
For more information call our Medford office at (541) 770-2020 or our Grants Pass office at (541) 956-2020.
Oregon Retina Center
Medford
1518 E Barnett Rd
Medford, OR 97504
(541) 770-2020
Write us a review
Grants Pass
1867 Williams Hwy
Grants Pass, OR 97527
(541) 956-2020
Write us a review
Contact
Monday, Tuesday, Wednesday, & Friday: 7:45 AM - 6:00 PM
Thursday: 7:45 AM - 5:00 PM
info@oregonretina.com
Proudly Serving Southern Oregon Communities
Jackson County, Josephine County, Applegate, Ashland, Butte Falls, Central Point, Cave Junction, Eagle Point, Grants Pass, Jacksonville, Lake Creek, Medford, Merlin, Murphy, Phoenix, Prospect, Provolt, Rogue River, Ruch, Sams Valley, Shady Cove, Sunny Valley, Talent, Trail, White City, Williams, Wolf Creek